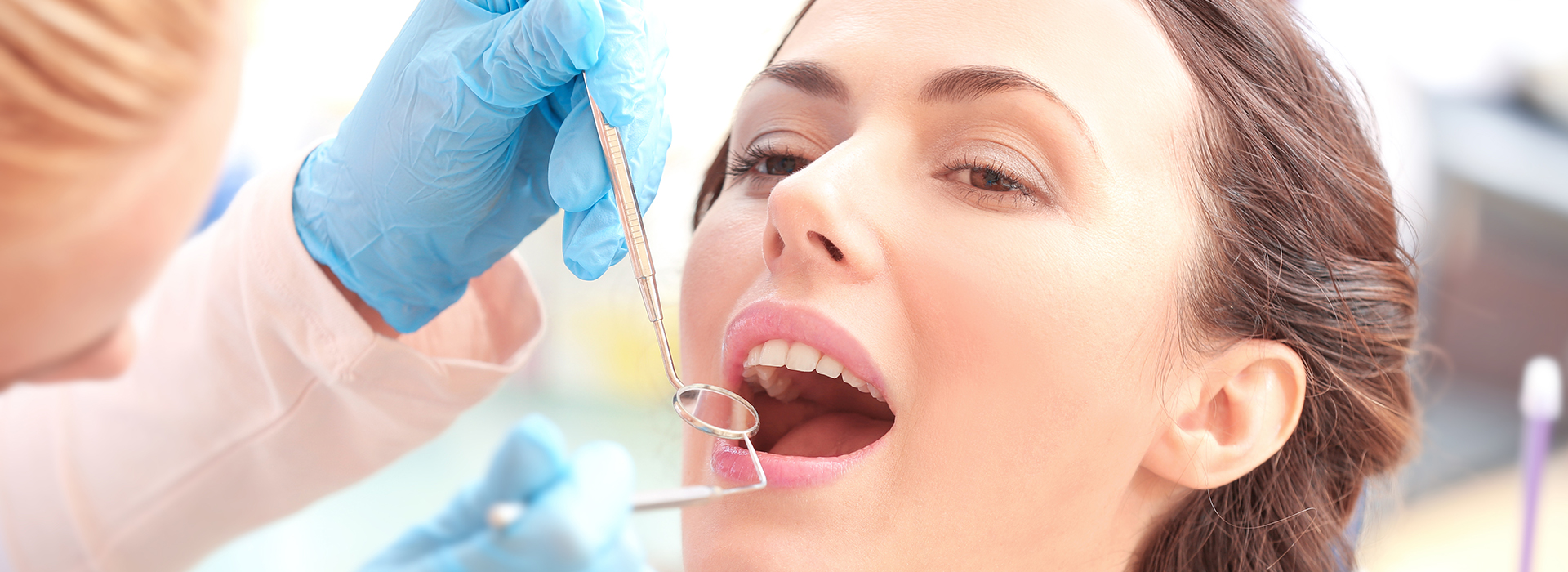
Gum disease is the leading cause of adult tooth loss in the United States, but it doesn’t have to be inevitable. Research from national health authorities shows periodontal conditions affect a large portion of adults, yet many instances can be prevented or managed when detected early. At the office of Silsby Family Dental, we focus on clear explanations, careful diagnosis, and practical care plans so patients understand their options and can protect both their smiles and long-term health.
Periodontal disease — commonly called gum disease — is an inflammatory response to bacteria that build up around the teeth and beneath the gumline. When plaque and tartar accumulate, the body reacts; the persistent inflammation can damage the soft tissues and the bone that support teeth. That process, left unchecked, is what leads to loosening teeth and eventual tooth loss.
Because early stages are often subtle, many people don’t recognize a problem until changes become noticeable. Regular dental exams and professional cleanings reveal early warning signs that might be missed at home, allowing for intervention before tissue damage becomes extensive.
Understanding the mechanics of periodontal disease — how bacteria, your immune response, and oral hygiene interact — is the first step toward meaningful prevention. Educated patients make the best partners in care, and our goal is to equip you with the knowledge to reduce risk and preserve lasting oral health.
Common signs that indicate a problem with your gums:
Gums that are swollen, tender, or visibly red rather than a healthy pink
Bleeding during or after brushing and flossing, even with gentle care
Gum recession exposing more of the tooth or root surfaces
Increased sensitivity to hot and cold or a persistent bad taste or breath
Teeth that feel loose, new gaps between teeth, or changes in how dentures fit
Pain when biting or signs of discharge near the gumline

Oral health does not exist in isolation. Increasing evidence links chronic gum inflammation to systemic conditions such as cardiovascular disease, diabetes, and respiratory concerns. While researchers continue to explore direct cause-and-effect relationships, controlling periodontal inflammation is a sensible step toward reducing overall health risks.
Good periodontal care supports better outcomes for patients with certain medical conditions, especially when those conditions are regulated in partnership with a primary care provider. Addressing gum disease is part of a broader approach to health that considers lifestyle, medical history, and preventive strategies.
At our practice, we emphasize prevention and early detection because stopping disease early reduces the need for invasive treatment later. Simple, consistent habits combined with professional oversight are the most efficient ways to maintain gum health and protect your general well-being.
Gingivitis is the earliest, most treatable stage of gum disease. It’s characterized mainly by inflammation of the gum tissue without the loss of bone supporting the teeth. Typical signs include redness, swelling, and bleeding during daily oral care. When addressed promptly, gingivitis can usually be reversed with non-surgical treatment and improved home care.
A professional evaluation confirms the diagnosis and helps rule out other causes of gum symptoms. Treatment at this stage often includes a thorough cleaning to remove plaque and hardened deposits, targeted advice on brushing and flossing technique, and a personalized schedule for maintenance visits.
Because gingivitis rarely causes pain, the condition frequently goes unnoticed. That is why regular dental checkups are critical: they let clinicians identify early inflammation and intervene before deeper tissues and bone are affected.

If gingivitis is not treated, it can progress to periodontitis — a stage where the inflammatory process damages the connective tissues and bone that hold teeth in place. As pockets form between the tooth and gum, bacteria find deeper hiding places that are harder to clean. Over time, this leads to recession, bone loss, and the potential for tooth mobility.
Managing periodontitis focuses on stopping destructive activity and stabilizing the supporting structures. Depending on severity, treatment may involve more frequent professional cleanings, localized antimicrobial therapies, or procedures to reduce pocket depth and restore healthy tissue contours.
Early and appropriate treatment improves the chance of preserving natural teeth and reduces the need for more complex interventions later. A staged approach — from conservative care to surgical options if required — lets patients and clinicians balance effectiveness, comfort, and long-term outcomes.
The choice of treatment depends on the stage of disease, the amount of tissue loss, medical considerations, and the patient’s goals. Non-surgical care, such as scaling and root planing, removes plaque and tartar from below the gumline and smooths root surfaces so tissue can reattach. These procedures are often combined with improved home care and targeted antimicrobial measures.
When deeper pockets persist or bone loss is significant, surgical approaches may be recommended to clean the roots thoroughly, reshape tissue, and, when appropriate, regenerate lost bone. Today’s surgical techniques can include flap procedures, regenerative grafts, and selective use of laser technology to enhance outcomes and reduce recovery time where applicable.
The overall goal is to restore a healthy environment for the gums and tooth-supporting structures and to make maintenance practical for daily home care. With regular follow-up and a commitment to oral hygiene, many patients maintain stable, comfortable results for years.
For early or moderate disease, non-surgical therapy is often the first line of treatment. Scaling and root planing remove bacterial deposits from below the gumline and help reduce pocket depth. When combined with improved daily hygiene and periodic maintenance cleanings, this approach can arrest disease progression and restore healthier gum attachment.
Adjunctive therapies — such as locally delivered antimicrobials or short courses of systemic medication in select cases — may be used to reduce bacterial load and support healing. The emphasis is on using the least invasive methods necessary to return the mouth to a stable, manageable state.
Patients who commit to an individualized home-care routine and a recommended recall schedule typically enjoy the best long-term results from conservative therapy.
When pockets are too deep for non-surgical measures alone or when bone loss requires reconstruction, surgery can improve access for cleaning and create conditions that support tissue regeneration. Pocket reduction (flap) surgery, guided tissue regeneration, and bone grafting are procedures designed to restore form and function where possible.
Modern techniques emphasize predictable healing and patient comfort. For certain procedures, lasers may be used to precisely remove diseased tissue and reduce bacterial populations. The team will review what to expect during recovery and how to care for the surgical site to support the best possible outcome.
Surgical care is paired with a long-term maintenance plan so improvements are preserved. Close communication between clinician and patient is essential to sustain oral health after treatment.
At Silsby Family Dental, our approach to periodontal care blends evidence-based techniques with clear, patient-centered communication. Whether the focus is prevention, stopping early disease, or reconstructive therapy, we design plans that respect your needs and long-term oral health goals.
If you have questions about gum health, notice any of the signs described above, or want to learn more about the treatment options we provide, please contact us for more information. Our team is ready to help you understand your condition and take the next steps toward a healthier smile.
Most people don’t realize that periodontal disease is the leading cause of tooth loss among adults. According to statistics from the Centers for Disease Control and Prevention, one out of every two adults over the age of 30 in the United States has periodontal disease.
You may be surprised to learn that the human mouth is home to a wide variety of microbes. The fact is that over 700 different strains of bacteria have been detected in the oral cavity. Although some of these bacteria are beneficial, others are harmful to oral health. Without proper oral hygiene and routine dental care, these harmful bacteria can cause tooth decay and gum disease, compromising both your oral health and overall wellbeing.
In addition to inadequate oral hygiene and infrequent professional care, other factors, including smoking, genetic tendencies, and unchecked diabetes, can contribute to the escalation of periodontal disease.
Your gums and teeth have an interdependent relationship, which means healthy teeth depend on the support of healthy gums. Also, taking care of your smile does more than keep your teeth and gums in optimal condition; good oral health also supports systemic health. In addition to being the leading cause of tooth loss in adults, researchers are finding more and more links between periodontal disease and a number of medical problems, including heart disease, stroke, diabetes, respiratory problems, and adverse pregnancy outcomes such as pre-term and low birth-weight babies.
If you notice that your gums are bleeding with the slightest pressure while brushing or flossing, it’s a sign of gingivitis. Although gingivitis is the earliest stage of gum disease, it can easily be reversed with deeper cleanings as well as an improved regimen of oral hygiene at home.
In the absence of professional treatment and better home care, gingivitis progresses to the next stage, which is known as periodontitis. In this stage, the connective tissue and bone that hold the teeth in place begin to break down with an increase in pocketing between the teeth and bone, gum recession, and bone loss. Without proper treatment by your dentist, periodontitis will progress from a mild to moderate loss of supporting tissue to the destruction of the bone around the teeth.
Although gingivitis can often be reversed with improved oral hygiene and professional cleanings, as periodontal disease advances, more extensive procedures are required to halt its progression. Based on a complete assessment of your periodontal health and a review of possible contributing factors, our office will recommend the best options in care. Treatment for periodontitis may include a series of deeper cleanings known as root planing and scaling, surgical procedures to reduce pocket depth, bone or tissue grafts, laser procedures, or antimicrobial medications.
The cost of care depends on the type of procedures required to restore your periodontal health. If you have dental insurance, plans often cover treatment to prevent gum disease as well as many procedures to treat the various stages of gum disease. Our goal is to help patients restore and maintain good oral health. We do all we can to help you begin care without additional stress or delay. Our business office works with you to maximize your benefits and provide easier, more convenient payment options.
By seeing our office regularly for care and doing your best to eat a healthy diet and practice good oral hygiene, you can keep your smile in tip-top shape as well as protect your overall wellbeing.
At the office of Silsby Family Dental, we provide a comprehensive range of services to address all your oral healthcare needs. You can rest assured that your smile is in the best of hands at our office. Our skilled and experienced team maintains a position at the forefront of advances in care and remains dedicated to providing the highest quality of skilled and compassionate treatment.