Tooth loss affects many adults at different stages of life and can influence eating, speech, and self-confidence. Fortunately, advances in implant dentistry now offer predictable, long-lasting solutions that mimic natural teeth in appearance and function. Our approach focuses on restoring not just a tooth, but the full experience of comfort, chewing ability, and a confident smile.
Dental implants act as a stable foundation for single crowns, multi-tooth restorations, and even full-arch replacements. They integrate with the jawbone to create a secure base that supports prosthetic teeth without relying on neighboring teeth for support. This stability preserves facial structure and helps avoid the gradual bone loss that follows missing teeth.
At Silsby Family Dental, we emphasize individualized care: evaluating each patient’s oral health, preferences, and lifestyle to recommend the implant solution that best meets their long-term goals. Our team combines clinical expertise with modern diagnostics to ensure treatment is both comfortable and tailored to your needs.

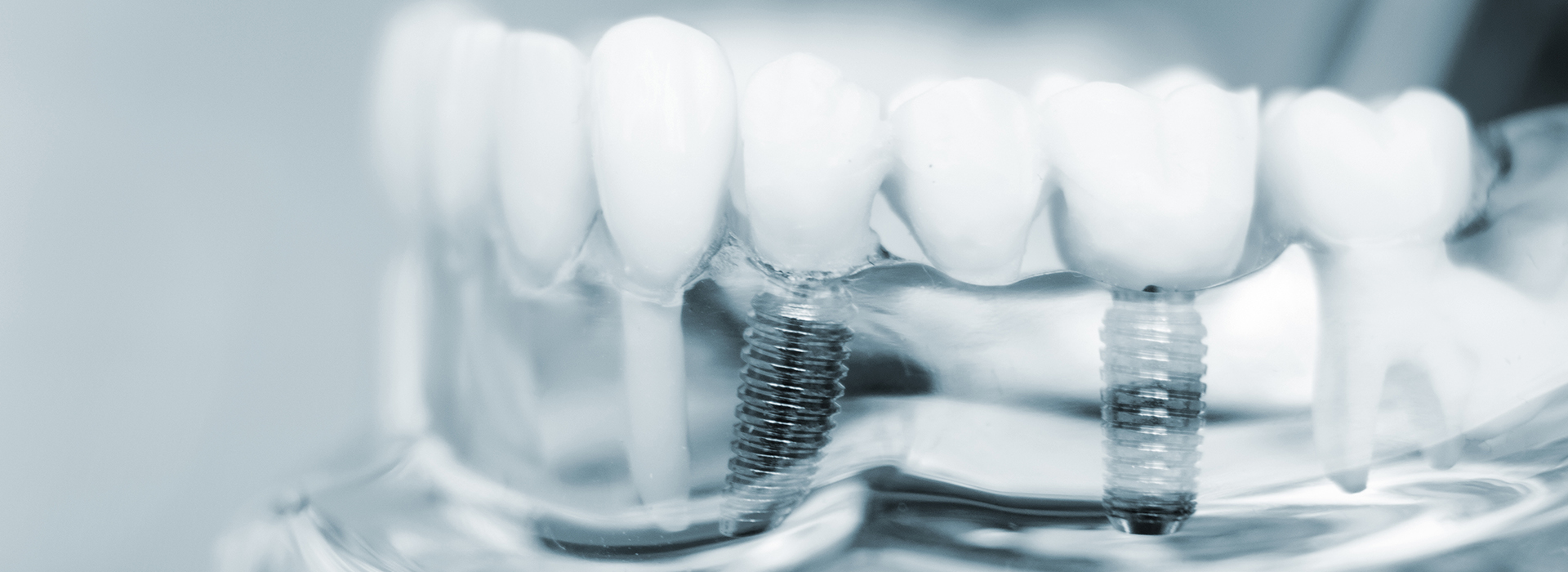
Dental implants are small, biocompatible posts that replace the root portion of a missing tooth. When placed in the jaw, they fuse with surrounding bone through a process called osseointegration, forming a durable platform for crowns, bridges, or denture systems. This root-level support is what sets implants apart, allowing replacement teeth to behave much like the originals.
Because implants anchor prosthetics directly to the bone, they deliver superior chewing stability and reduce the risk of slipping or movement that can occur with removable dentures. Patients commonly report improved confidence when speaking and eating, since implant-supported restorations feel secure and predictable.
Beyond function, implants also contribute to long-term oral health. They help maintain jawbone volume by transmitting forces to the bone during chewing, which discourages the resorption that often follows tooth loss and helps preserve natural facial contours.
Most dental implants are crafted from titanium or other biocompatible materials that the body readily accepts. After surgical placement, the surrounding bone begins to remodel and integrate with the implant surface, creating a stable union. This biological bond is the key to the implant’s long-term success and ability to support various types of restorations.
The timeline for integration varies with the location of the implant, the quality of the bone, and individual healing patterns. Some patients receive temporary restorations immediately after placement, while others follow a staged approach that allows fuller healing before the definitive prosthesis is attached. Your treatment plan will reflect the option that best balances predictable healing with your aesthetic and functional goals.
Compared with removable dentures or conventional bridges, dental implants offer several notable benefits. They replicate the mechanical behavior of natural teeth closely, allowing for a wide range of foods to be enjoyed without concern for slippage. Their stability also reduces the need to alter healthy adjacent teeth, which is often necessary when fabricating fixed bridges.
Implants can last many years with careful oral hygiene and routine dental care. Because they help preserve bone and support facial tissues, implants contribute to a more youthful facial profile over time. For many patients, these functional and aesthetic benefits make implants the preferred long-term solution for tooth replacement.
Beyond comfort and appearance, implants simplify day-to-day care: implant-supported crowns and bridges can be brushed and flossed much like natural teeth, and implant-retained dentures can be designed to be either removable for cleaning or fixed for added convenience.
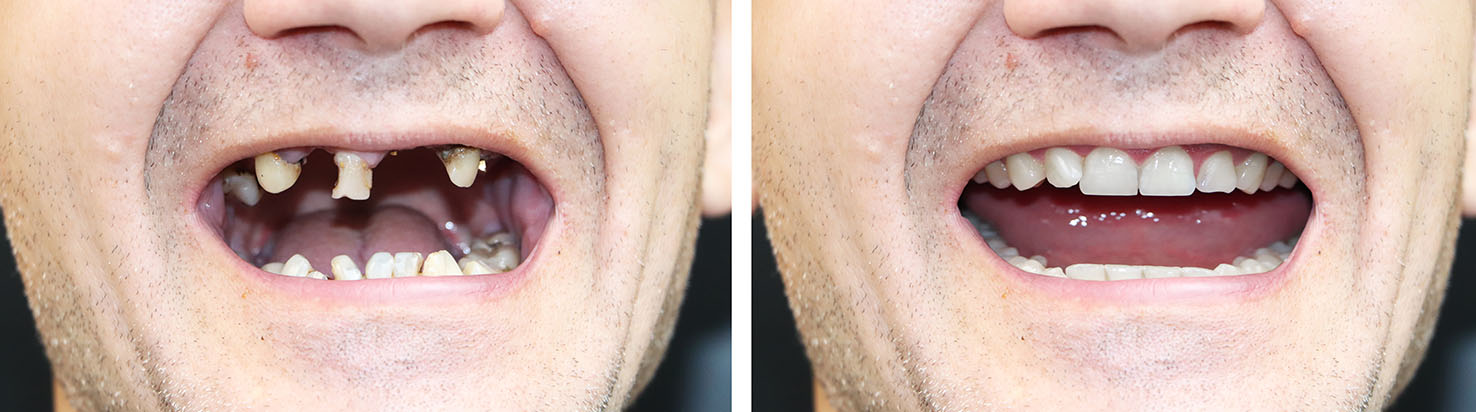
Most adults who are free of uncontrolled medical conditions and who have sufficient jawbone can pursue implant therapy. Key factors in candidacy include oral health, bone volume, the presence of periodontal disease, and lifestyle habits such as tobacco use. A thorough clinical exam and diagnostic imaging allow us to evaluate these elements and recommend appropriate preparatory procedures when needed.
For patients with limited bone, procedures such as bone grafting or sinus augmentation can often create adequate support for implants. We assess each patient’s anatomical needs and discuss alternatives so you can make an informed choice that aligns with your expectations.
Your overall health and any medications you take will also factor into treatment planning. Our team develops personalized plans that reflect your dental history, restorative goals, and long-term oral health strategy.
The implant journey begins with a comprehensive consultation: a review of your medical and dental history, clinical examination, and detailed imaging such as cone-beam CT when indicated. These diagnostic steps allow precise planning of implant placement in three dimensions and help us design restorations that harmonize with your bite and facial appearance.
Surgical placement is typically performed under local anesthesia, with sedation options available for patient comfort. The actual procedure is often straightforward and performed on an outpatient basis. After placement, the implant must integrate with the bone—a process that can take several months. During this phase, temporary restorations may be used to maintain function and aesthetics.
Once osseointegration is complete, impressions are taken to fabricate the final crowns, bridges, or implant-supported dentures. These prostheses are carefully adjusted for function and comfort, with the goal of achieving a natural appearance and a balanced bite. We emphasize clear communication at every step so you understand what to expect from placement through final restoration.
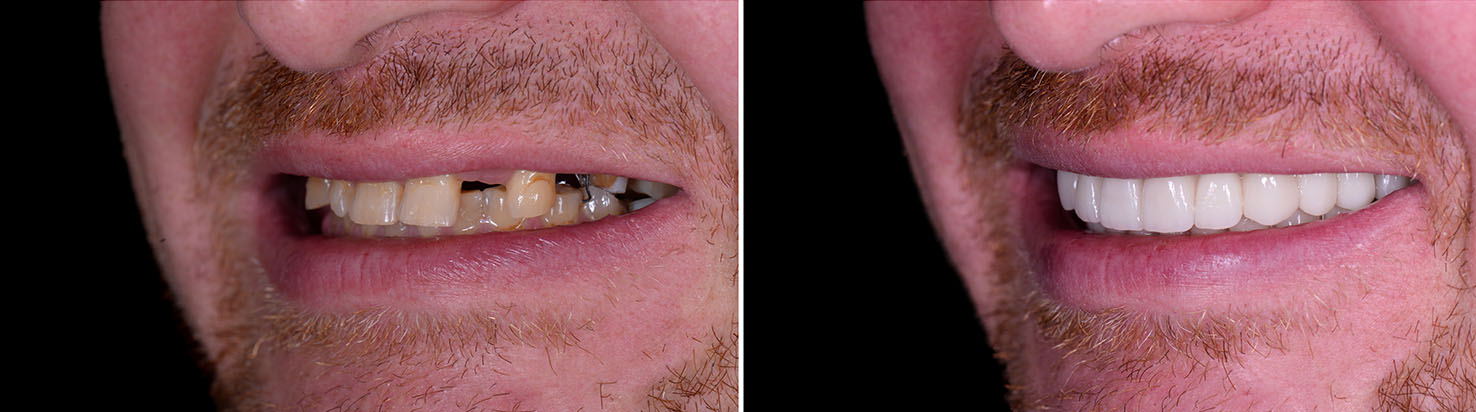
Successful implant placement depends on having adequate bone to support the implant. When bone has diminished after tooth loss or periodontal disease, grafting procedures can rebuild volume and create a stable foundation. Bone grafts use either donor material or the patient’s own bone to encourage new bone formation in the area of the implant.
Sinus lifts, ridge augmentation, and socket preservation are common techniques to address specific anatomical challenges. These procedures have become routine in implant dentistry and are performed with predictable outcomes when indicated. The need for grafting is determined during the diagnostic phase and explained as part of your individualized treatment plan.
Healing timelines vary, and your care team will outline realistic expectations for the grafting and implant phases. Our goal is to ensure that any preparatory work supports a durable, functional final restoration.
Dental implants are a durable solution when supported by good oral hygiene and regular professional care. After restoration, ongoing maintenance includes routine dental checkups, periodic radiographic evaluations, and conscientious home care. While implants are resistant to decay, the surrounding tissues remain susceptible to inflammation and infection if not properly maintained.
We take pride in helping patients through each stage of implant therapy and in providing clear guidance for long-term preservation of their restorations. If you would like to explore implant dentistry further and see how it might restore comfort and confidence to your smile, contact us for more information. Our team is happy to discuss options and answer your questions.
If you've lost a tooth due to injury, decay, gum disease, or any other reason, we recommend dental implants to replace missing teeth. Dental implants come the closest to replicating the look, feel, and function of your natural teeth.
Dental implants are placed into the jawbone and mirror the same function as the root of a tooth. The procedure for dental implants is usually performed while a patient is sedated. Patients who undergo IV sedation must have an empty stomach and transportation home following the procedure. Most sedation patients will have little to no memory of the procedure occurring.
Generally, dental implants are made out of a biocompatible metal such as titanium. Biocompatible metals are also used for other common bone implants (such as shoulder, hip, and knee replacements). The visible portion of the implant is usually made out of porcelain and is custom-made to match your existing teeth.
Dental implants are designed to fuse to the bone, which makes them become permanent fixtures. Typically speaking, the success rate is nearly 100%. There are few cases in which the implant will not fuse as intended and must be removed. If this happens to occur, the procedure can be attempted again a few months later.
Dental implants are not usually covered by dental insurance, but may be covered under a patient's medical insurance. Our office and your insurance company can discuss coverage options with you based on your individual case and treatment plan.
It's easy... just take care of an implant as if it's a natural tooth! This involves regular brushing, flossing, and dental checkups. If you have any concerns about your implant, contact us immediately.